CHSU Simulation Center
STANDARDIZED PATIENT/ Participant PROGRAM

Thank you for your interest in our Standardized Patient/Participant program in the College of Osteopathic Medicine Simulation Center at California Health Sciences University (CHSU).
We are currently hiring!
About the Standardized patient/Participant program
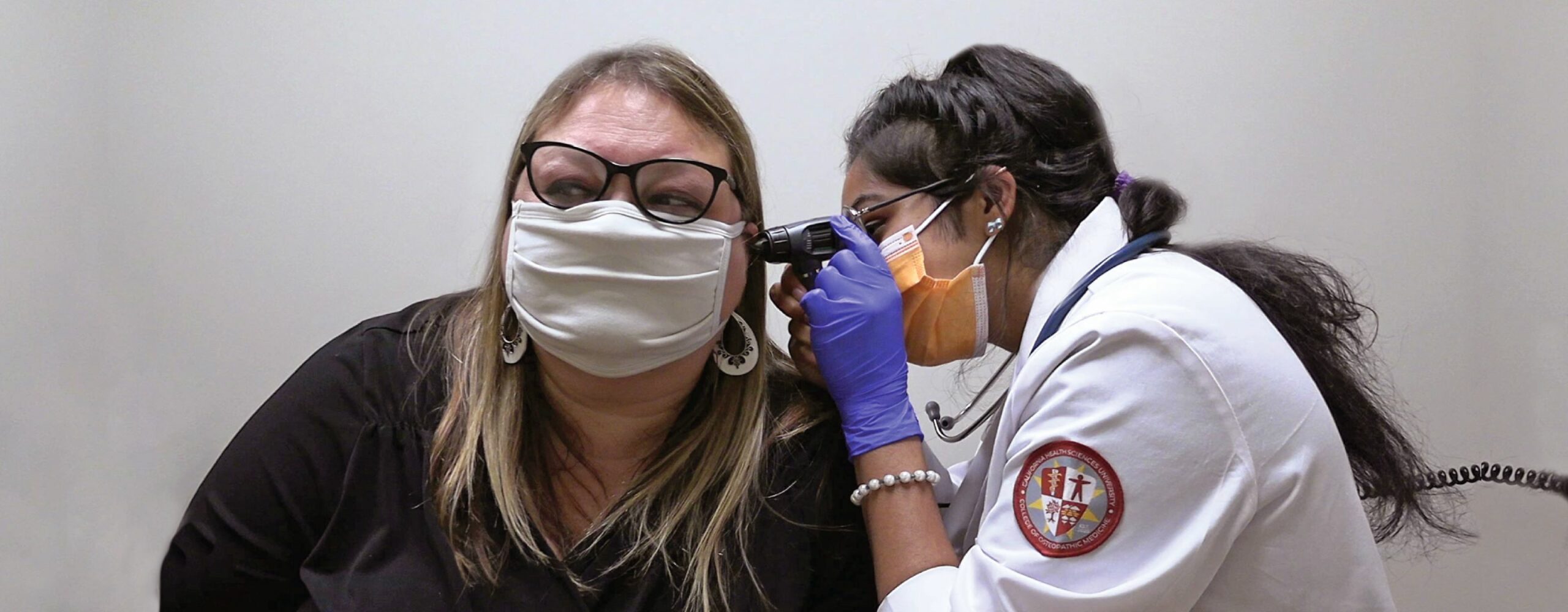
Standardized Patients/Participants (SPs) are individuals who can help provide direct, hands-on patient care experiences. Drawing from their diverse backgrounds and skills, SPs enjoy a flexible work schedule and contribute to the development of health care professionals.
SP simulation involves specifically trained individuals to portray the roles of patients, family members or others. Because of this training, it allows learners to practice physical exam skills, history taking, communication, and other exercises. SPs are trained to consistently and accurately portray specific emotions, behaviors and disease symptoms. This includes accurately relaying personal and medical history with everyday concerns while interacting with learners during simulated patient experiences.
SPs are also involved with giving responsive feedback to a learner’s performance during assessment experiences, so good memory and observation skills are a must. Some of the patient encounters do require learners to perform physical exams, however, invasive physical examinations or procedures are not allowed. For more information please see FAQs below.
Minimum Qualifications
Qualifications and qualities to become an SP include:
- Reliable and punctual
- Good memory and recall skills
- Excellent communication and interpersonal skills
- Ability to work with others
- Committed to the education of health care professionals
- Professionalism in interactions
- Keeping information confidential
- Be willing to learn
- Ability to easily adapt
- Positive attitude
- No biases toward gender, race, religion, national origin, or physical characteristics
- Comfortable with physical exam simulations
- Accurate completion of a medical database questionnaire to help match the SP to the appropriate patient cases (some real-life medical conditions or histories may conflict with simulated patient cases).
No previous experience is required.
SPs are only utilized on an “as needed” basis, with time commitments occurring Monday through Friday between 7:30am – 12pm or 12:30pm – 5pm. While scheduling is planned each year, there is no guaranteed number of hours and some requests may be made on short notice.
Frequently Asked questions
The simulation experience provides students with a safe and highly effective learning environment and can be either for practice or an exam, both of which are important educational opportunities for students. Repetitively portraying a specific patient role in the same, standardized way for multiple students keeps the evaluations fair and unbiased. This requires concentration while being interviewed and examined, each time. At the conclusion of the simulation, you must recall the student’s performance to evaluate them on the checklist and possibly give verbal feedback.
Standardized patients are required to attend orientation and will receive foundational training on basic SP skills, including patient portrayal and student evaluation. Prior to every SP experience, SPs will attend case training and may be asked to participate in practice sessions with the Simulation Center staff.
No. SPs come from various backgrounds, and we will teach SPs the assigned roles.
We will provide the SP with a complete patient history to learn. The history includes the patient’s complaint for which he/she comes to see the doctor, his/her past medical history, and details about his/her life such as employment, family, and activities. We also will provide the SP with an emotional state he/she is in during the encounter. By learning that history, the SP can learn to portray the patient and speak to the doctor. The SP also is taught how to move like the patient and how to react to the physical examination. For example, an SP may be portraying someone with a bad back. The SP is then shown the location of the pain on his/her body and what the patient could or could not do because of the back problem.
Yes. Students are informed that they will be working with SPs but are instructed to behave as though SPs are real patients.
Standardized Patients may be asked to complete a checklist as a record of the encounter and also give verbal constructive feedback on communication skills.
Students will perform focused physical examinations based on the patient case as they would with a real patient. The students will not perform the following physical examinations: breast, pelvic, genital or rectal exams, nor will they perform invasive procedures, such as drawing blood or throat cultures.
SPs will be asked to wear a patient gown for realism. Under this gown, the SP should wear some sort of sports clothing (shorts, sports bra) as students will place the stethoscope directly on their chest.
Yes. Students and SPs should not do anything that might be harmful. SPs are just portraying someone who has a medical condition. The examinations are very basic and do not cause any harm to the SP. If an SP had cause for concern, he/she would be entitled to stop an examination.
Yes, an SP can pass on a role that they do not want to portray.
No. The SP patient portrayal information will contain all information needed.
If an SP is familiar with or related to a student, they will not be scheduled as a patient for that simulation experience.
Yes, it is important. If there are significant positive findings during a simulated physical exam, it could confuse the student. However, a surgical scar might not matter, or it could be written into the patient’s case. Yet, a surgical scar on an appendectomy patient will disqualify that patient to be an appendectomy patient. An SP’s answers on the medical database questionnaire will help match the SP to the appropriate patient cases.
A wide range of skills help in selecting an SP. The ability to communicate effectively is important. Being comfortable with a wide variety of people in differing situations is valuable. Being able to express feedback verbally and in writing is extremely important for the student. Punctuality, reliability and flexibility are imperative.
No. Some SPs are trained and experienced actors, but most are not. You can be a very good SP without acting experience. There are some similarities to what actors do, but there are differences, too.
This is a part-time, hourly position, reporting on an as needed basis. There is no guarantee for the number of hours worked.
The number of days and hours worked are not guaranteed or consistent. It will depend on the particular exam and usually be a 4-5 hour session in a day.
The hourly pay rate will be discussed during the interview.
Apply
If you are interested in becoming an SP, please apply by submitting the online application and a detailed resume to apurewal@chsu.edu when completed.
Interview Process
The interview process is as follows:
- Your application and resume will be reviewed to ensure you meet minimum qualifications.
- Given you meet the qualifications, you will have a personal Zoom interview with Simulation Center staff to:
- Determine suitability for becoming an SP
- Answer questions
- After the Zoom interview, selected applicants will be invited to the CHSU Simulation Center for an audition.
As an employee of CHSU, reference and background checks are necessary before a formal offer can be made to be hired as a CHSU SP.
For more information, please contact Anand Purewal Ray, Standardized Participant Learning and Development Trainer, at apurewal@chsu.edu
